|
Post-operative courseJessica was admitted to the PICU at 2255 hours, accompanied by two anaesthetists, two perfusionists, an OR nurse and Odim. She was extremely pale and her extremities were cool. She had severe fluid retention-her body had retained an additional 1,280 millilitres of fluid while on bypass. The admitting nurse, Colleen Kiesman, recorded that Jessica's face was so swollen (another sign of fluid retention) that she could not open Jessica's eyes to check her pupils. Jessica continued to experience bleeding problems throughout her stay in the PICU. Her urine had blood in it, and there was continuous bloody oozing from her sternum, which was a sign of a coagulopathy or clotting disorder. Coagulopathy problems can arise when a patient has been on bypass for a long time. Blood cells react differently when pushed through a bypass machine, as opposed to when they are normally pumped by the heart through the lungs. Thus, a lengthy bypass can damage the patient's blood cells and limit their ability to clot. For this reason, a wound that would normally clot quickly can turn into a serious site of bleeding following a prolonged period on bypass. Because ECMO is a type of bypass machine, it can also interfere with blood clotting. On Friday, Jessica was still on ECMO, which was being operated by a perfusionist. She had continued to bleed from her chest into special drainage tubes. (Chest tubes are inserted post-operatively to drain fluid or air from around the lungs, thus allowing the lungs to expand.) While the blood drained through the chest tubes, the tubes were not the cause of the bleeding. That day, Jessica lost 525 millilitres of blood in six hours. To compensate for this loss, she was given blood transfusions. A chest X-ray showed that her edema and atelectasis were improving, but an echocardiogram showed that her heart was deteriorating. Jessica had increased left atrial and ventricular enlargement, decreased septal motion and a residual VSD shunt. In an attempt to find a source of bleeding, Odim re-explored Jessica's chest in the PICU on Saturday at 2325 hours. He reported that she had a generalized coagulopathy, some leaking of blood from around the aortic cannula site (to which he added a second suture), and some blood within the mediastinum (the space around the top of the heart in the chest). The blood loss from the chest tubes continued to be enormous. Jessica lost a total of 2,732 millilitres in 24 hours. Numerous transfusions of blood and blood products were given. On Sunday, March 27 there was still significant oozing of blood where the lines entered Jessica's body. The sternotomy site also continued to ooze, and the chest tube losses totalled 1,220 millilitres of blood over six hours. This means that over a 30-hour period, she lost eight times her blood volume. Odim was concerned about the lack of improvement in her ongoing coagulopathy. He considered it unlikely that her condition would improve while she remained on ECMO. Indeed, the longer she remained on the machine, the worse were her chances of recovery. Odim decided to wean her from ECMO in the PICU, a decision that Kesselman agreed with, since Jessica was in too fragile a state to be moved to the OR. The decision to perform the procedure in the PICU was risky. In his testimony, Kesselman said that it had been never successfully done in the unit. In her testimony, Feser said that the PICU nursing staff were not familiar with weaning from ECMO or decannulating lines, one of the steps of the weaning process. "It is not something that you do on a basis of, you know, very short notice." (Evidence, page 29,947) The cardiac bins that the PICU staff had asked Odim to help them prepare were still not ready, as Odim had not yet responded to the request for a list of equipment. Kesselman said that there was no discussion of requesting OR nursing assistance. Hancock scrubbed in to act as Odim's assistant, while Kesselman and other PICU nurses were to perform essential monitoring functions. A perfusionist, Dave Smith, was present and continuing to provide perfusion services for the ECMO. There was no anaesthetist present, although an anaesthetist's presence is required by policy for all surgical procedures at the HSC. Weaning from ECMO would appear to be a surgical procedure. An anaesthetist would have been able to provide assistance with ventilation, monitoring and relieving pain, providing other medications and treating blood problems. Weaning Jessica from the ECMO machine should have been done in a more organized fashion, with a properly prepared surgical team. Odim seems to have failed to appreciate that fact. He proceeded without ensuring that there was appropriate staff in place to assist in the procedure. He did not direct that appropriately trained nurses be called in, although the evidence established that this assistance was available if requested. The evidence suggested that once the procedure to remove Jessica from the ECMO machine started, matters quickly grew chaotic and critical. Jessica had been losing considerable amounts of blood before the procedure, and her condition was already badly compromised by her steady deterioration after the operation. On removal of the inferior vena cava cannula, Jessica experienced a sudden and massive loss of blood. According to Odim and Hancock, the blood loss occurred through the opening at the cannula site. Odim could not staunch the flow of blood quickly or adequately. At Jessica's bedside there were no Satinsky clamps (the type of clamp that is best suited for clamping such openings in a blood vessel). One of the ICU staff was sent to the OR supply room to get one. This took minutes to accomplish, during which time Odim attempted to decrease the loss of blood by pressing his fingers against the cannula opening. Once the clamp arrived, Odim attempted to suture the site closed, but with the already-heavy loss of blood, his efforts proved futile. Jessica died before he could close the site completely. Had Odim responded earlier to Feser's request for a list of equipment he needed in the PICU, the proper clamps would likely have been in place. The request for the clamps might also have alerted the PICU staff to the fact that Odim intended to undertake such procedures in the PICU. Jessica was a small child. The available evidence established that the total amount of blood in her system would have been about 500 millilitres (half a litre). It would not have taken very long for her body to drain itself of all of its blood through a sustained opening such as a cannula site, in the absence of adequate pressure on the site. However, what went unnoticed during the procedure was the fact that either the surgeon or his assistant had failed to clamp the inferior vena cava cannula line after removing it from Jessica. It is quite possible that Jessica bled to death through this unclamped line. In the normal procedure for weaning a patient from bypass or ECMO, the surgeon announces that he or she is going to remove a venous cannula. At this point, the perfusionist will clamp the venous cannula line at the pump. The surgeon is expected to clamp the line at the patient's end. 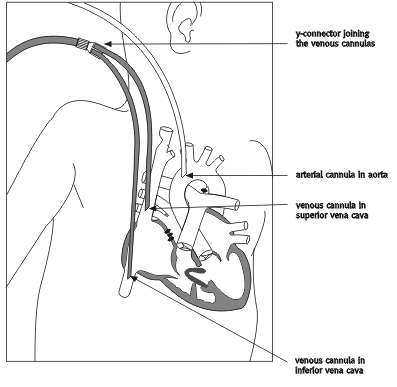 Diagram 6.5 - Depiction of the connection of the ECMO Odim did not clamp the line. This was an error for a number of reasons. Air can enter the unclamped line and, ultimately, the machine and then the patient, if it is necessary to go back on bypass. Blood that is in the line can be lost since it will simply drain out of the line. Finally, there is the danger that the patient can bleed to death. This danger arises from the fact that the lines from the inferior vena cava and the superior vena cava are joined together by what is termed a Y connector. From this connector, blood flows through a single line to the ECMO machine. If, as happened in this case, the line from the inferior vena cava is decannulated, while the line to the superior vena cava remains cannulated, blood can continue to flow from the child into the line from the superior vena cava. However, that blood can no longer flow into the ECMO machine if, as happened (quite appropriately) in this case, the line has been clamped at the ECMO end of the line. Instead, the blood can simply drain out of the unclamped line that had been connected to the inferior vena cava. Perfusionist Dave Smith testified that once he heard a member of the team announce that the cannula had been removed, he noted a dramatic increase in the volume of blood he needed to transfuse into Jessica to maintain her pressure. He started to run out of blood to transfuse. "This was happening very quickly, the nurses were bringing blood from the blood bank, albumin. I was adding clear fluid just to keep going, keep the pressure up." (Evidence, page 9,803) According to Smith, someone gave the order to go back on ECMO. Smith said he responded that he had no blood left. "And after that, at that point, they decided to quit I believe." (Evidence, page 9,804) Jessica went into cardiac arrest during this period. She could not be resuscitated and was pronounced dead at 1216 hours on March 27, 1994. While Odim went to speak to the family, Smith went to look at the child's body. At that point, I noticed a venous cannula lying on the bed, beside the baby's chest. It was unclamped. I found that unusual, so I asked-Dr. Hancock was still there. She was across Jessica from Jonah and Murray Kesselman was at the head of the bed. I asked if this had ever been clamped, was this clamped at one time? And they said they didn't think so. They couldn't recall it being clamped. And they wanted to know why, so I proceeded to explain the physics of the situation. (Evidence, page 9,805) Smith said that next to the cannula there was a flannel sheet that was soaked with blood. In her testimony, Hancock stated that Odim took the cannula out and handed it to her. At that time Jessica started to bleed seriously. I remember thinking, you know, that it wasn't clamped. But at the same time, the big problem was inside where she was bleeding from the inferior vena cava, and it was really just welling right up. (Evidence, page 20,648) For this reason she said that she and Odim both turned their attention to the bleeding they could see. It was during this period that a nurse was sent for the Satinsky clamp. Odim testified that it was Hancock, not himself, who removed the cannula, under his instruction. He also testified that he was in the process of closing the bleeding site without a clamp. Odim testified that he heard the sound of the siphoning of blood from the heart and noted the decline in the heart's power. At that point he said he recognized that there could not be a clamp on the line. He concluded the major blood loss was from the cannula. Odim stated that the line was then clamped. He testified: I don't recall who placed the clamp, whether Dr. Hancock placed it or myself. I just said, listen, we have to get a clamp on the line, and a clamp was got, and the line was clamped, the SVC cannula was clamped. I don't recall whether I did it or B.J. did it. We were sort of looking for a Kelly clamp and the clamp got applied. (Evidence, pages 24,205-24,306) From Smith's testimony, it appears that Hancock might not have understood the dangers of not clamping the line. An experienced OR nurse might have noticed if the line was unclamped. However, the ICU nurses were not used to, or trained in, operating-room procedures, especially the procedures related to removal of a patient from bypass. Smith did not complete an incident report about the event. In his testimony he indicated that he believed incident reports to be essentially a nursing responsibility. Smith was, however, quite upset by these events and reported them to Maas, his supervisor. Maas spoke with Odim the following day. He told Odim of the dangers in not clamping the line and the need to conduct these procedures in a manner that allowed the perfusionist a clear view of the lines. In his testimony, Maas said of Odim: He acknowledged that a mistake had been made. He was quite straightforward and up front about it and that it wouldn't happen in the future and things would be done in orderly fashion. (Evidence, page 6,932) Maas said that he did not fill out an incident report on the matter because: We are not that familiar with incident reports, I will be quite honest. We don't fill them out because there are no incidents with us that we have ever experienced up to this point. Obviously this is an incident, and we felt the best route to go was a direct route. (Evidence, page 6,932) It should be noted that the filing of incident reports did not preclude also speaking with Odim. Odim's account of post-operative discussions differs considerably from the evidence provided by Smith and Maas. I ventilated a little bit at the bedside when I recognized at the end that things weren't done as smoothly as things could have been done. Those were sort of my discussions with my team members at the bedside. I don't recall a later discussion with Mike. It's certainly possible that I might have had some words with him. Q. Do I infer from your use of the word "ventilate" that you were angry with them? Odim: At the whole, as I said I think there was a little bit of a break down, and I-nobody was sort of looking at the monitor, and we didn't know when the blood pressure was dropping from the monitor. We were all there. I said well, I am sitting tying a knot and trying to control bleeding, somebody needs to tell us, yell out what's going on, and that didn't happen very efficiently. I was a little concerned that there was a delay to put the clamp on and asked my assistant, when you take the cannula out, don't you always clamp it, and why wasn't that done? And I also, I asked Mr. Smith, that, you know, if the blood pressure goes down, you need to let us know so we go right back on ECMO. So, that was sort of the discussion I had with my team members as, you know, the person in charge to facilitate so that this would not happen again. (Evidence, pages 24,208-24,209) In later testimony, Odim was presented with Maas's testimony to the effect that he had spoken to Odim about the incident and that in a straightforward manner Odim had acknowledged that a mistake had taken place. Odim said: "Unfortunately I don't recall the specifics of that conversation." (Evidence, page 24,243) In his patient progress notes, Odim wrote that he had successfully weaned Jessica from ECMO with stable cardiac functions, although inotropic drugs were being administered, for approximately forty minutes. He wrote that she then developed severe bleeding following removal of the inferior vena cava cannula. Odim said that she was placed back on ECMO but could not be stabilized. This report does not capture the confused nature of events. This statement was also contradicted by Dave Smith, who said that Jessica was never successfully re-established on ECMO. None of the medical staff made an entry in this child's chart indicating that a clamp had not been placed on the IVC venous cannula line, despite the clear importance that this would have had in determining the cause of the baby's death. This omission is a glaring one and bears comment. As noted in Chapter Three the chart or medical record is a crucial source of information. Failure to chart pertinent events would, for example, prevent the Chief Medical Examiner's office from reaching an appropriate conclusion as to whether or not an inquest should be held into a child's death. Additionally, the medical record is a primary source of information for the family of a deceased child. The HSC as a matter of policy in these cases made the charts available to the families of the children who died in 1994. In this case, anyone reading the Ulimaumi chart would not have been able to determine what occurred in the PICU during the attempt to wean Jessica from the bypass machine, since not all of the material facts were disclosed in the chart. When asked why the clamp issue was not mentioned, Odim said: I think the operative report states what happened in terms of the destabilization of the patient during decannulation. (Evidence, page 24,215) On that point Odim was not correct. The operative report gives little indication of the events disclosed by the evidence.
|
| Current | Home - Table of Contents - Chapter 6 - Post-operative course |
| Next | Autopsy findings |
| Previous | The operation-March 24 |
| Section 1 | Chapter 1 - Introduction to the Issues |
| Chapter 2 - Pediatric Cardiac Issues | |
| Chapter 3 - The Diagnosis of Pediatric Heart Defects and their Surgical Treatment | |
| Chapter 4 - The Health Sciences Centre | |
| Section 2 | Chapter 5 - Pediatric Cardiac Surgery in Winnipeg 1950-1993 |
| Chapter 6 - The Restart of Pediatric Cardiac Surgery in 1994 January 1, 1994 to May 17, 1994 |
|
| Chapter 7 - The Slowdown May 17 to September 1994 |
|
| Chapter 8 - Events Leading to the Suspension of the Program September 7, 1994 to December 23, 1994 |
|
| Chapter 9 - 1995 - The Aftermath of the Shutdown January to March, 1995 |
|
| Section 3 | Chapter 10 - Findings and Recommendations |
| Appendix 1 - Glossary of terms used in this report | |
| Appendix 2 - Parties to the Proceedings and counsel | |
| Appendix 3 - List of witnesses and dates of testimony | |
| Diagrams | |
| Tables | |